Pelvic Floor Training for Women: Exercises, Benefits and Tips
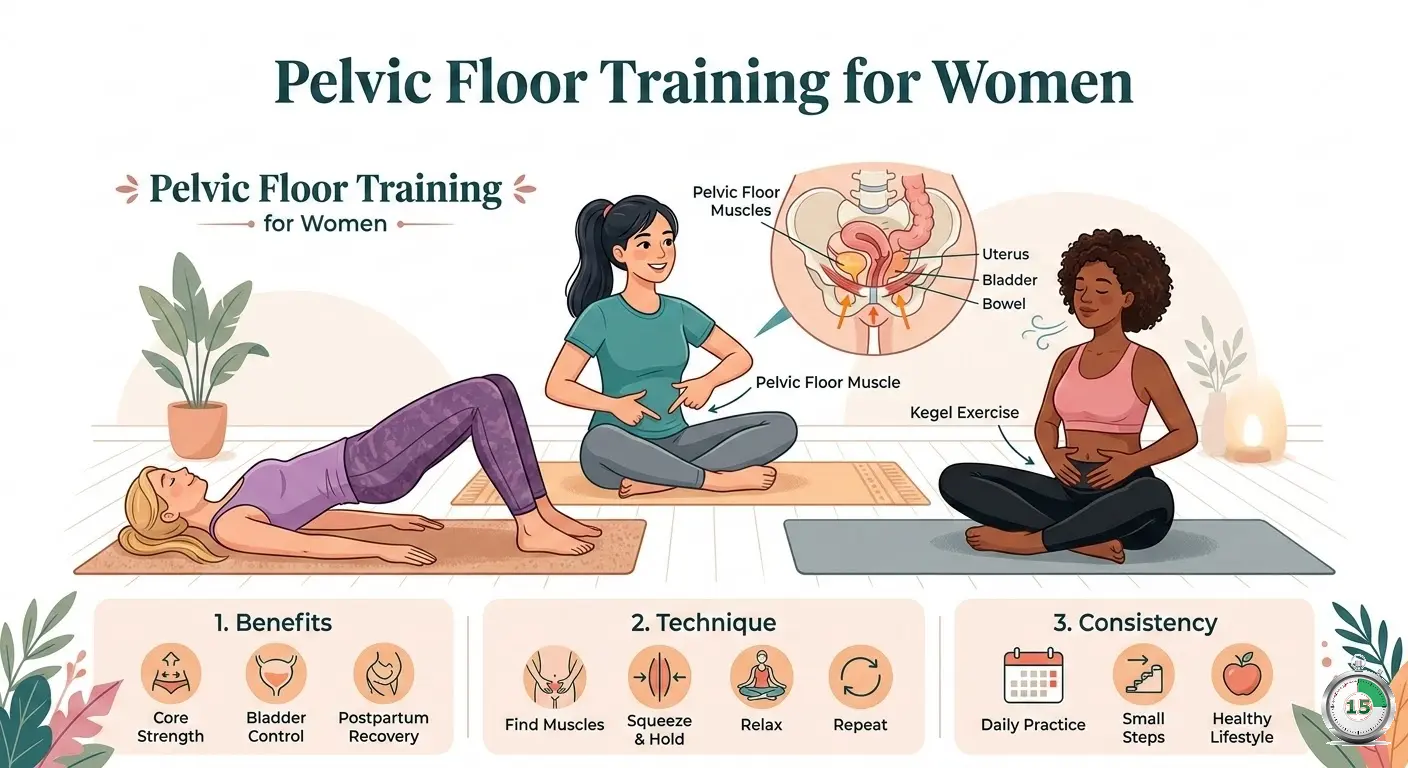
Most exercise programs target the muscles you see. The pelvic floor, the group of muscles that make up the base of the pelvis, is rarely included but plays an important role in bladder control, spinal stability, and sexual function.
For women in particular, these muscles endure a lot of stress from pregnancy, childbirth, hormonal changes, and high-impact exercise. Training them is not optional. It is important.
This guide covers anatomy, the best exercises, and what to do when training alone doesn’t fully solve the problem.
What is the Pelvic Floor?
The pelvic floor is a layered group of muscles and connective tissue that extends across the base of the pelvis like a hammock. It supports the bladder, uterus, and intestines.
These muscles control continence, influence spine and hip stability, and play a direct role in sexual arousal. If they are weak or dysfunctional, symptoms range from mild leakage to chronic pelvic pain.
Both hypotonic (too weak) and hypertonic (too strong) pelvic floor can cause problems. The right training method depends on the situation.
Pelvic Floor Exercises
Kegel Exercises
Kegels are the foundation of pelvic floor exercises. Contract the muscles you use to stop the flow of urine, hold for 5 to 10 seconds, and then release completely. Aim for 3 sets of 10 repetitions every day.
According to the Mayo Clinic, a consistent Kegel practice can significantly reduce stress incontinence and improve muscle tone within 4 to 8 weeks of regular training.
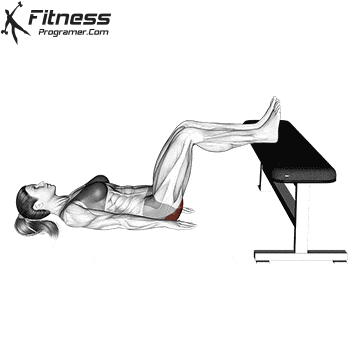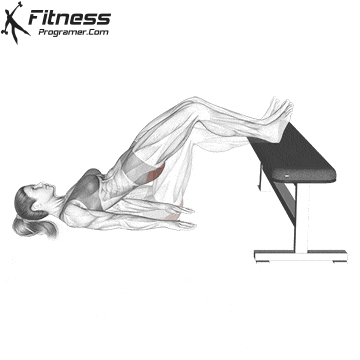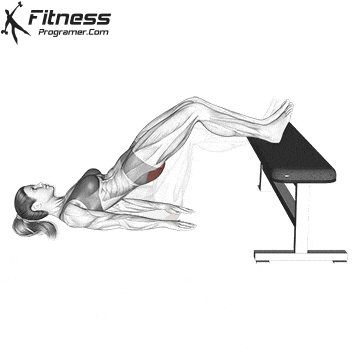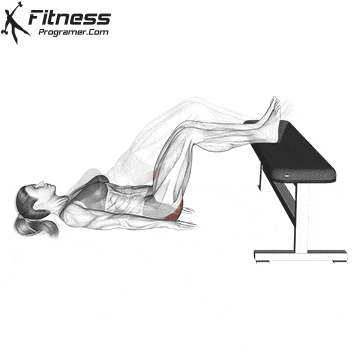
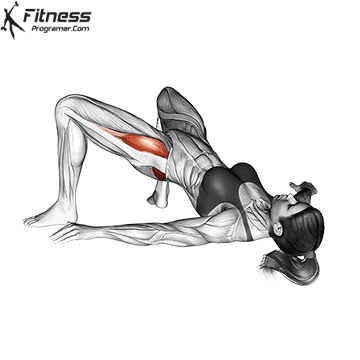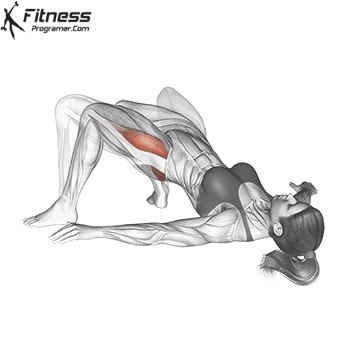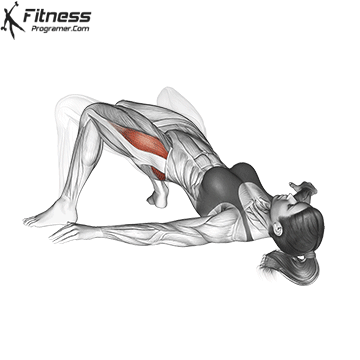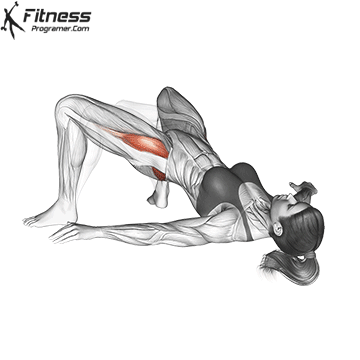
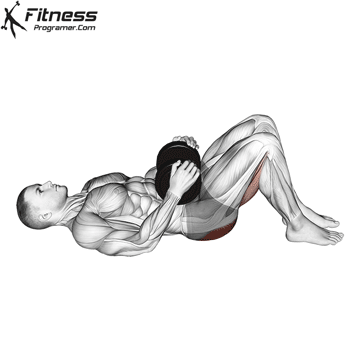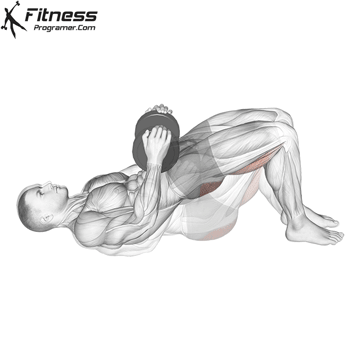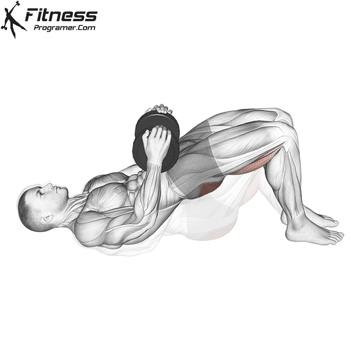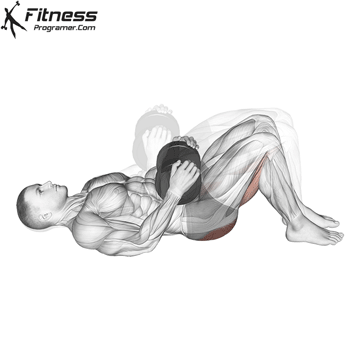
Glute Bridges
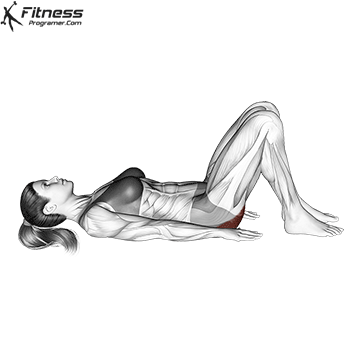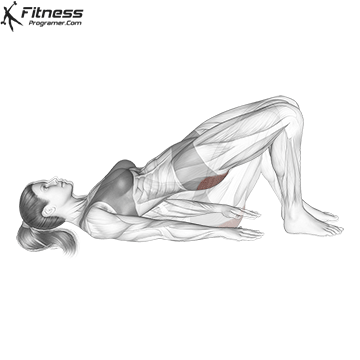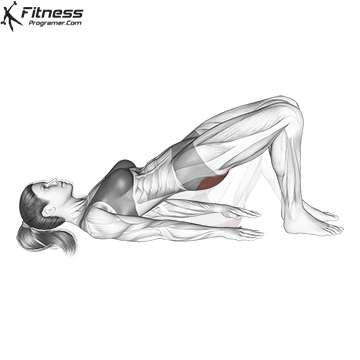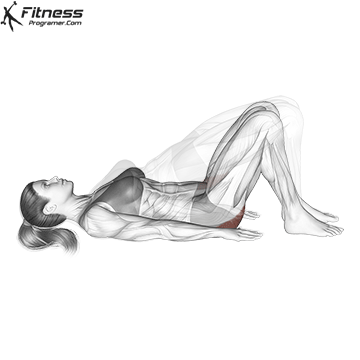
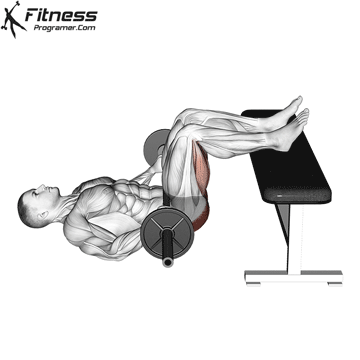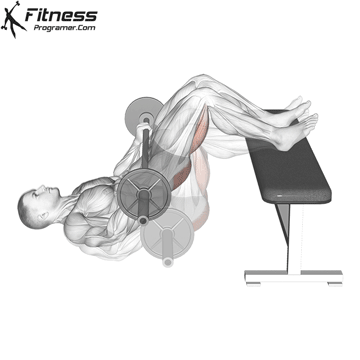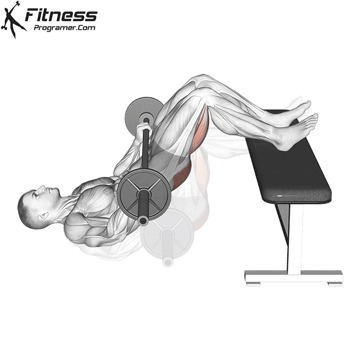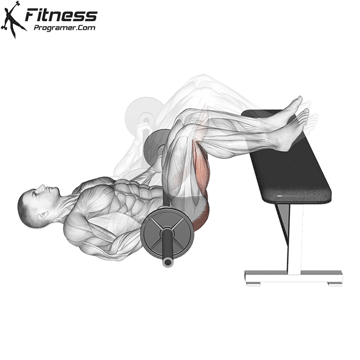
Lie on your back with your knees bent and your feet facing the floor. Engage your pelvic floor, and press through your heels to lift your hips to the ceiling. Hold for 2 to 3 seconds at the top before lowering.
This exercise targets the pelvic floor alongside the glutes and hamstrings, making it one of the most effective lower body movements for overall pelvic health.
Changes:
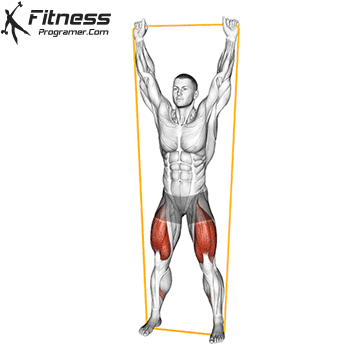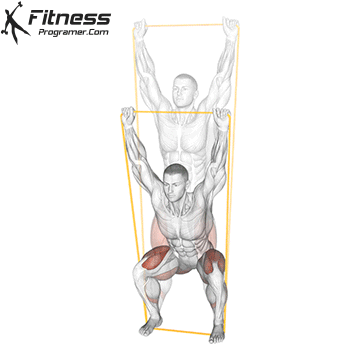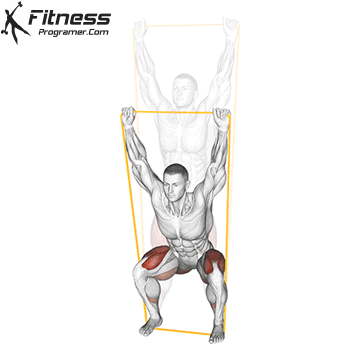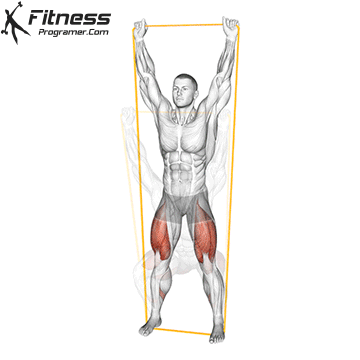
Squats
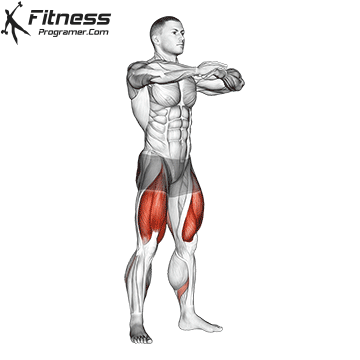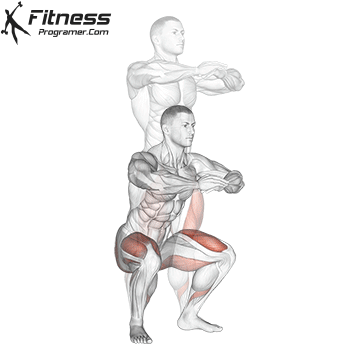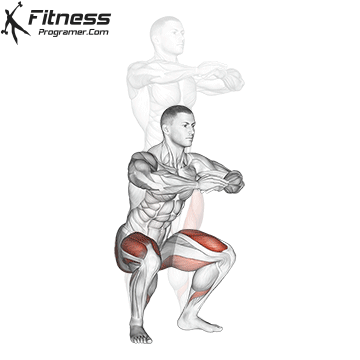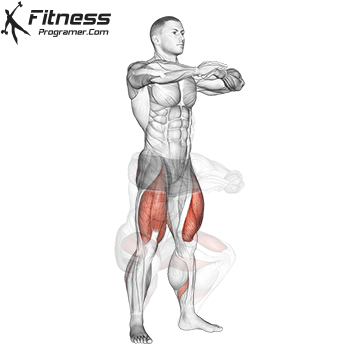
Controlled squats strengthen the entire pelvic region. Stand with feet shoulder-width apart, engage your core and pelvic floor, and lower yourself until your thighs touch the floor.
Focus on a full release at the bottom and controlled compression on the way up. Avoid rapid movements, as pelvic floor activity requires intention.
Changes:
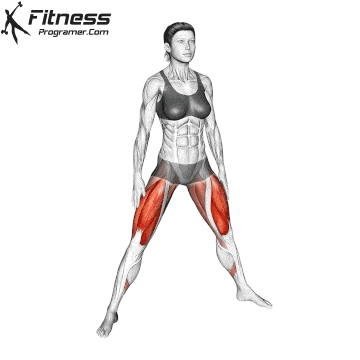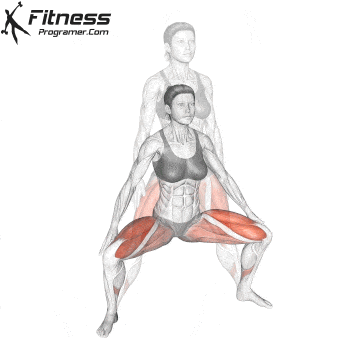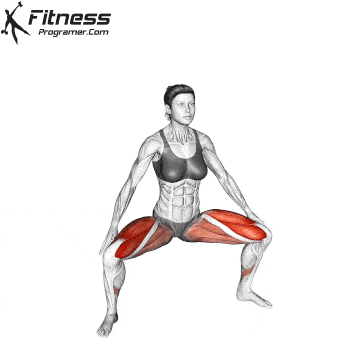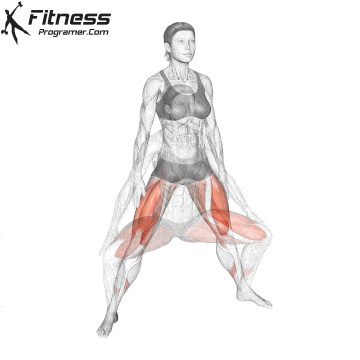


Pelvic Tilts
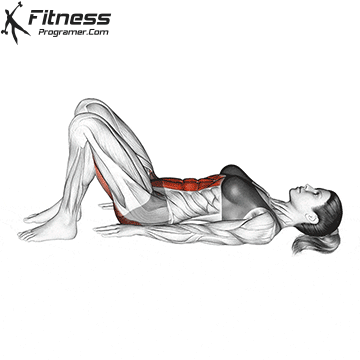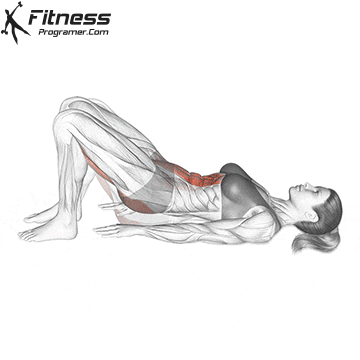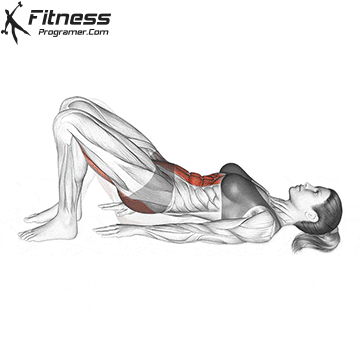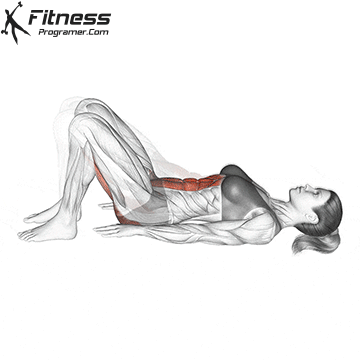
Lie on your back with your knees bent. Gently flatten your lower back by tilting your pelvis up. Hold for 5 seconds before releasing. This movement works the deep core and pelvic floor together.
Training vs. Clinical Options: A Comparison
Exercise is basic, but some conditions require more support. Here’s how the main methods compare.
| The way | Difficulty | Time to See Results | It’s very good |
| Kegel exercises | The beginner | 4 to 8 weeks | Minor leaks, basic tone |
| Pelvic tilts and bridges | The beginner | 4 to 6 weeks | Spinal and pelvic stability |
| Squats (controlled) | The middle one | 6 to 10 weeks | Total pelvic strength |
| Pelvic floor PT sessions | Guided therapy | 8 to 12 weeks | Dysfunction, prolapse, pain |
| Non-surgical rehabilitation | Clinical process | 1 to 3 times | Looseness, dryness, sensitivity |
Results are highly dependent on exercise consistency, proper technique, and the underlying cause of the dysfunction. If symptoms persist after 8 to 12 weeks of regular training, a clinical evaluation is recommended.
When Exercise Is Not Enough
For some women, exercise alone does not fully resolve looseness, dryness, or sensitive anxiety, especially after giving birth or during menopause when hormone levels drop dramatically.
Pelvic floor physiotherapy offers biofeedback-guided training and individualized goals that go beyond what conventional exercises can achieve at home.
For those facing significant tissue changes, non-surgical options are also available. Women in the tri-state area can explore female genital rejuvenation in New Jersey with board-certified specialists who provide radiofrequency and laser-based treatments with no downtime.
These therapies address tissue tone, softening, and sensitivity and are increasingly being used alongside pelvic floor therapy as a complementary approach.
What the Experts Say
Marcy Crouch, PT, DPT, a board-certified women’s health specialist, recommends that women begin pelvic floor training before problems arise, noting that preventive training is much easier than rehabilitation after significant inactivity.
The American Urogynecologic Society lists pelvic floor muscle training as the first clinical recommendation for stress incontinence, with evidence supporting its effectiveness in all age groups.
Many experts advise learning proper technique under supervision before attempting independent high-volume training, as incorrect Kegel technique is more common than many think.
Scientific Perspectives on Kegel Exercises
Several studies confirm the effectiveness of Kegel exercises:
- Frequency and intensity: A 2006 study emphasized that programs lasting three months or more yield the best results. Cavkaytar et al. suggested at least eight weeks as the minimum time for visible improvement.
- Sexual Health: Research shows that regular Kegel exercises can improve orgasmic power, arousal, and satisfaction in women, including postmenopausal women.
- Quick Results: Other studies, such as those by Messe et al., report sexual arousal
Frequently Asked Questions
How often should I do pelvic floor exercises?
Most guidelines recommend 3 sets of 10 repetitions at least 3 times a day. Consistency is more important than volume. Daily practice brings better results than occasional periods of high repetitions.
Can pelvic floor exercises improve sex drive?
Yes. Stronger pelvic floor muscles are associated with improved sexual sensation and satisfaction. A study published in the journal Neurourology and Urodynamics supports this connection.
How do I know if I’m doing Kegels correctly?
Contractions should feel like lifting and squeezing, not bending down. If you are unsure, a pelvic floor physiotherapist can guide you using biofeedback at the same time.
Should I stop high impact exercise if I have pelvic floor problems?
That’s not the case. Changing the intensity and volume can help. A pelvic floor specialist can advise on which movements to continue, modify, or temporarily avoid based on your specific presentation.
Are non-surgical treatments a substitute for exercise?
No. Clinical treatment addresses tissue-level changes that cannot resolve. Exercise remains the cornerstone of long-term pelvic floor health, with clinical options as a supplement when needed.
More from FitnessProgramer
For guided exercise resources, check out the hip exercises and abs and core workout sections on FitnessProgramer, which include movements that specifically support pelvic health and spine stability.
Final thoughts
The pelvic floor deserves a place in every woman’s training program. It is an active muscle group, and like any other, it responds to consistent, well-done work.
Start with the basics, train with purpose, and don’t ignore symptoms that persist beyond a few months of regular practice.
If exercise has its limitations, appropriate clinical support is available. Knowing both options puts you in control of your pelvic health
References:
- Andrew L Siegel: Pelvic floor muscle training in men: practical applications
- Grace Dorey and friends: Pelvic floor exercises for erectile dysfunction
- Pelvic floor exercises for the treatment of post-micturition dribble in men with erectile dysfunction: a randomized controlled trial.



